Understanding and Managing Acne Vulgaris: Causes, Symptoms, Types and Treatment Options
DOI:
https://doi.org/10.5530/ajphs.2026.16.90Keywords:
Acne, Propionibacterium acnes, Acne causes, Acne types, Acne treatmentAbstract
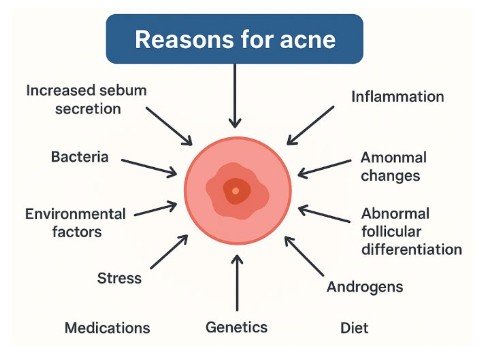
Acne is a common skin condition that affects millions of individuals worldwide, causing physical and psychological distress. This article aims to provide an overview of the causes, symptoms, different types of acne and their respective treatments. The causes of acne vulgaris are multifactorial, involving an increase in sebum secretion, bacteria, inflammation, hormonal changes, androgens, genetics, diet, medicine, cosmetics, stress, environmental factors, and lifestyle factors. The types of acne discussed include non-inflammatory lesions, also called comedones, which include blackheads and whiteheads. Inflammatory lesions include pustules, papules, nodules, and cysts. Various treatment options, particularly topical and oral medications, are available for acne vulgaris. Topical treatments, such as benzoyl peroxide, salicylic acid, retinoids, and antibiotics, are commonly used for mild to moderate acne. For more severe cases, oral medications like antibiotics, isotretinoin, and hormonal therapy can be used. Hormonal therapy, such as a combination of oral contraceptives and anti-androgens, is recommended primarily for female patients. The effectiveness of each treatment method varies depending on the type and severity of acne, as well as individual patient factors such as skin type, age, hormonal status, and treatment tolerance. By understanding the distinct characteristics of each acne type and the available treatment options, healthcare professionals can make up-to-date decisions and tailor treatment plans to meet the specific needs of patients.
References
Abdulla, H., & Shalita, A. (2009). Topical clindamycin preparations in the treatment of acne vulgaris. Expert Review of Dermatology, 4(2), 155–162. https://doi.org/10.1586/edm.09.3
Adalatkhah, H., Pourfarzi, F., & Sadeghi, B. (2011). Flutamide versus a cyproterone acetate-ethinyl estradiol combination in moderate acne: A pilot randomized clinical trial. Clinical, Cosmetic and Investigational Dermatology, 4, 117–121. https://doi.org/10.2147/CCID.S20543
Agarwal, S., & Agarwal, S. (2019). Pharmacology For Undergraduates (3rd ed.). CBS Publishers & Distributors.
Akhavan, A., & Bershad, S. (2003). Topical Acne Drugs: Review of Clinical Properties, Systemic Exposure, and Safety. American Journal of Clinical Dermatology, 4(7), 473–492. https://doi.org/10.2165/00128071-200304070-00004
Alamdari, N., Tavakolian, K., Alhashim, M., & Fazel-Rezai, R. (2016). Detection and classification of acne lesions in acne patients: A mobile application, 2016 IEEE International Conference on Electro Information Technology (EIT), 0739–0743. https://doi.org/10.1109/EIT.2016.7535331
Alexandre Rocha, M., Sousa Costa, C., & Bagatin, E. (2014). Acne vulgaris: An inflammatory disease even before the onset of clinical lesions. Inflammation & Allergy-Drug Targets (Formerly Current Drug Targets-Inflammation & Allergy)(Discontinued), 13(3), 162–167.
Almazrouei, B., Islayem, D., Alskafi, F., Catacutan, M. K., Amna, R., Nasrat, S., Sizirici, B., & Yildiz, I. (2023). Steroid hormones in wastewater: Sources, treatments, environmental risks, and regulations. Emerging Contaminants, 9(2), 100210. https://doi.org/10.1016/j.emcon.2023.100210
Alturki, R., Albishri, M., Alharbi, R., Meeralam, R., Alanazi, S., Alsayary, A., & Alzahrani, K. (2023). Knowledge and Awareness about the teratogenic effects of oral Isotretinoin among women in Saudi Arabia. Medical Science, 27(132), e110ms2901. https://doi.org/10.54905/disssi/v27i132/e110ms2901
Ambizas, E., & Sousonis, F. (2016). Acne Vulgaris: Different OTC treatments. US Pharmacist, 41(11), 7–11. https://www.uspharmacist.com/article/acne-vulgaris-different-otc-treatments
Angelette, A. L., Rando, L. L., Wadhwa, R. D., Barras, A. A., Delacroix, B. M., Talbot, N. C., Ahmadzadeh, S., Shekoohi, S., Cornett, E. M., Kaye, A. M., & Kaye, A. D. (2023). Tetracycline-, Doxycycline-, Minocycline-Induced Pseudotumor Cerebri and Esophageal Perforation. Advances in Therapy, 40(4), 1366–1378. https://doi.org/10.1007/s12325-023-02435-y
Arooj, A., Rehman, A. U., Iqbal, M., Naz, I., Alhodaib, A., & Ahmed, N. (2023). Development of adapalene loaded liposome based gel for acne. Gels, 9(2), 135. https://doi.org/10.3390/gels9020135
Aydemir, E. H. (2014). Acne vulgaris. Turkish Archives of Pediatrics/Türk Pediatri Arşivi, 49(1), 13–16. https://doi.org/10.5152/tpa.2014.1943
Babaeinejad, S., Khodaeiani, E., & Fouladi, R. F. (2011). Comparison of therapeutic effects of oral doxycycline and azithromycin in patients with moderate acne vulgaris: What is the role of age? Journal of Dermatological Treatment, 22(4), 206–210. https://doi.org/10.3109/09546631003762639
Baki, G. (2022). Introduction to cosmetic formulation and technology. John Wiley & Sons.
Barros, B., & Thiboutot, D. (2017). Hormonal therapies for acne. Clinics in Dermatology, 35(2), 168–172. https://doi.org/10.1016/j.clindermatol.2016.10.009
Basak, S. A., & Zaenglein, A. L. (2013). Acne and its management. Pediatrics in Review, 34(11), 479–497. https://doi.org/10.1542/pir.34-11-479
Baughman, R., & Valeyre, D. (2018). Epidemiology and Causes. In Sarcoidosis: A Clinician’s Guide (1st ed.). Elsevier Health Sciences.
Benner, N., & Sammons, D. (2013). Overview of the treatment of acne vulgaris. Osteopathic Family Physician, 5(5), 185–190. https://doi.org/10.1016/j.osfp.2013.03.003
Bettoli, V., Guerra-Tapia, A., Herane, M. I., & Piquero Martín, J. (2019). Challenges and Solutions in Oral Isotretinoin in Acne: Reflections on 35 Years of Experience. Clinical, Cosmetic and Investigational Dermatology, 12, 943–951. https://doi.org/10.2147/CCID.S234231
Beylot, C., Doutre, M. S., & Beylot-Barry, M. (1998). Oral contraceptives and cyproterone acetate in female acne treatment. Dermatology, 196(1), 148–152. https://doi.org/10.1159/000017849
Bhadra, P., & Atanu, D. (2020). A literature review on acne due to hormonal changes and lifestyle. Indian Journal of Natural Sciences, 10(59), 18507–18521.
Bienenfeld, A., Nagler, A. R., & Orlow, S. J. (2017). Oral Antibacterial Therapy for Acne Vulgaris: An Evidence-Based Review. American Journal of Clinical Dermatology, 18(4), 469–490. https://doi.org/10.1007/s40257-017-0267-z
Biggs, C. A. (2023). Effect of Skin Microbiota on Acne. Chancellor’s Honors Program Projects, University of Tennessee, Knoxville. https://trace.tennessee.edu/entities/publication/59dd5cec-6d2c-46e1-8a7e-f12bca930643
Bottomley, W. W., & Cunliffe, W. J. (1993). Severe flares of acne following isotretinoin: Large closed comedones (macrocomedones) are a risk factor. Acta Dermato-Venereologica, 73(1), 74–74. https://doi.org/10.2340/000155557374
Bowe, W. P., Joshi, S. S., & Shalita, A. R. (2010). Diet and acne. Journal of the American Academy of Dermatology, 63(1), 124–141. https://doi.org/10.1016/j.jaad.2009.07.043
Brown, S., & Shalita, A. (1998). Acne vulgaris. The Lancet, 351(9119), 1871–1876. https://doi.org/10.1016/S0140-6736(98)01046-0
Capitanio, B., Sinagra, J. L., Ottaviani, M., Bordignon, V., Amantea, A., & Picardo, M. (2009). Acne and smoking. Dermato-Endocrinology, 1(3), 129–135. https://doi.org/10.4161/derm.1.3.9638
Carlborg, L. (1986). Cyproterone Acetate Versus Levonorgestrel Combined with Ethinyl Estradiol in the Treatment of Acne: Results of a multicenter study. Acta Obstetricia et Gynecologica Scandinavica, 65(S134), 29–32. https://doi.org/10.3109/00016348609157049
Chanda, R., Poornima, T., & Vikas, S. (2013). Acne and its treatment lines. International Journal of Research in Pharmaceutical and Biosciences, 3(1), 1–16.
Charny, J. W., Choi, J. K., & James, W. D. (2017). Spironolactone for the treatment of acne in women, a retrospective study of 110 patients. International Journal of Women’s Dermatology, 3(2), 111–115. https://doi.org/10.1016/j.ijwd.2016.12.002
Chen, Y.-W., Chang, Y.-L., Wu, C.-Y., & Chen, Y.-J. (2023). Prevalence of acne in Taiwan: A 13-year population-based retrospective study. The Journal of Dermatology, 50(4), 568–570. https://dx.doi.org/10.1111/1346-8138.16709
Chilicka, K., Gold, M. H., & Nowicka, D. (2023). Acne vulgaris and the most popular and new cosmetological treatments. Journal of Cosmetic Dermatology, 22(7), 1946–1950. https://doi.org/10.1111/jocd.15757
Chu, S., Michelle, L., Ekelem, C., Sung, C. T., Rojek, N., & Mesinkovska, N. A. (2021). Oral isotretinoin for the treatment of dermatologic conditions other than acne: A systematic review and discussion of future directions. Archives of Dermatological Research, 313(6), 391–430. https://doi.org/10.1007/s00403-020-02152-4
Chularojanamontri, L., Tuchinda, P., Kulthanan, K., & Pongparit, K. (2014). Moisturizers for acne: What are their constituents? The Journal of Clinical and Aesthetic Dermatology, 7(5), 36. PMCID: PMC4025519
Clark, C. (2009). Acne: Causes and clinical features. Clinical Pharmacist, 1(4), 163–167.
Cliff, S., Pararajasingam, A., & Mathew, L. (2023). Cosmeceutical-Related Dermatitis and Allergies. In Essentials for Aesthetic Dermatology in Ethnic Skin (1st ed., pp. 143–148). CRC Press.
Common, J. E. A., Barker, J. N., & van Steensel, M. A. (2019). What does acne genetics teach us about disease pathogenesis? British Journal of Dermatology, 181(4), 665–676. https://doi.org/ 10.1111/bjd.17721
Conforti, C., Giuffrida, R., Fadda, S., Fai, A., Romita, P., Zalaudek, I., & Dianzani, C. (2021). Topical dermocosmetics and acne vulgaris. Dermatologic Therapy, 34(1), e14436. https://doi.org/10.1111/dth.14436
Cunha, B. A., Sibley, C. M., & Ristuccia, A. M. (1982). Doxycycline. Therapeutic Drug Monitoring, 4(2), 115. https://doi.org/ 10.1097/00007691-198206000-00001
Cunliffe, W. J., C’Otterill, J. A., & Williamson, B. (1972). The effect of Clindamycin in acne-a clinical and laboratory investigation. British Journal of Dermatology, 87(1), 37–41. https://doi.org/10.1111/j.1365-2133.1972.tb05095.x
Feneran, A., Kaufman, W., Dabade, Dabade, T., & Feldman, S. (2011). Retinoid plus antimicrobial combination treatments for acne. Clinical, Cosmetic and Investigational Dermatology, 4, 79–92. https://doi.org/10.2147/CCID.S13873
Dallo, M., Patel, K., & Hebert, A. A. (2023). Topical antibiotic treatment in dermatology. Antibiotics, 12(2), 188. https://doi.org/ 10.3390/antibiotics12020188
Daniele, S. G., Kim, S. R., Grada, A., Moore, A. Y., Suozzi, K. C., & Bunick, C. G. (2023). Truncal Acne and Scarring: A Comprehensive Review of Current Medical and Cosmetic Approaches to Treatment and Patient Management. American Journal of Clinical Dermatology, 24(2), 199–223. https://doi.org/ 10.1007/s40257-022-00746-4.
Das, S., & Reynolds, R. V. (2014). Recent Advances in Acne Pathogenesis: Implications for Therapy. American Journal of Clinical Dermatology, 15(6), 479–488. https://doi.org/10.1007/s40257-014-0099-z
Dawson, A. L., & Dellavalle, R. P. (2013). Acne vulgaris. British Medical Journal, 346, f2634. https://doi.org/ 10.1136/bmj.f2634
De Caux, D., Mariappa, G., Perera, G., & Girling, J. (2023). Prescribing for pregnancy: Chronic skin diseases. Drug and Therapeutics Bulletin, 61(4), 55–60. https://doi.org/10.1136/dtb.2022.000036
Del Rosso, J. Q., & Tanghetti, E. (2013). A status report on topical tazarotene in the management of acne vulgaris. Journal of Drugs in Dermatology, 12(3), s53-8. PMID: 23545935.
Drake, L., Reyes-Hadsall, S., Barbieri, J. S., & Mostaghimi, A. (2022). New Developments in Topical Acne Therapy. American Journal of Clinical Dermatology, 23(2), 125–136. https://doi.org/10.1007/s40257-021-00666-9
Dréno, B., Bettoli, V., Ochsendorf, F., Layton, A., Mobacken, H., & Degreef, H. (2004). European recommendations on the use of oral antibiotics for acne. European Journal of Dermatology, 14(6), 391–399. PMID: 15564203
Dréno, B., Layton, A., Zouboulis, C. C., López‐Estebaranz, J. L., Zalewska‐Janowska, A., Bagatin, E., Zampeli, V. A., Yutskovskaya, Y., & Harper, J. C. (2013). Adult female acne: A new paradigm. Journal of the European Academy of Dermatology and Venereology, 27(9), 1063–1070. https://doi.org/10.1111/jdv.12061
Du-Thanh, A., Kluger, N., Bensalleh, H., & Guillot, B. (2011). Drug-Induced Acneiform Eruption. American Journal of Clinical Dermatology, 12(4), 233–245. https://doi.org/10.2165/11588900-000000000-00000
Ebede, T. L., Arch, E. L., & Berson, D. (2009). Hormonal treatment of acne in women. The Journal of Clinical and Aesthetic Dermatology, 2(12), 16–22. PMID: 20725580
Elsaie, M. (2016). Hormonal treatment of acne vulgaris: An update. Clinical, Cosmetic and Investigational Dermatology, 9, 241–248. https://doi.org/10.2147/CCID.S114830
Fardet, L., Kassar, A., Cabane, J., & Flahault, A. (2007). Corticosteroid-Induced Adverse Events in Adults: Frequency, Screening and Prevention. Drug Safety, 30(10), 861–881. https://doi.org/10.2165/00002018-200730100-00005
Farrah, G., & Tan, E. (2016). The use of oral antibiotics in treating acne vulgaris: A new approach: Oral antibiotics for acne vulgaris: a new approach. Dermatologic Therapy, 29(5), 377–384. https://doi.org/10.1111/dth.12370
Farzam, K., Nessel, T. A., & Quick, J. (2023). Erythromycin. In StatPearls [Internet]. StatPearls Publishing.
Fathi, M. M., Diab, N. A., & Said Abdelshafy, A. S. (2023). Efficacy and Safety of Combination of Mometasone Furoate 0.1% Cream and Adapalene 0.1% Gel in Alopecia Areata. Zagazig University Medical Journal, 29(1.1), 319–323. https://doi.org/10.21608/zumj.2020.18821.1625
Feldman, S., Careccia, R. E., Barham, K. L., & Hancox, J. (2004). Diagnosis and treatment of acne. American Family Physician, 69(9), 2123–2130. PMID: 15152959
Ferensztajn-Rochowiak, E., & Rybakowski, J. K. (2023). Long-term lithium therapy: Side effects and interactions. Pharmaceuticals, 16(1), 74. https://doi.org/10.3390/ph16010074
Fernandez‐Obregon, A. C. (2000). Azithromycin for the treatment of acne. International Journal of Dermatology, 39(1), 45–50. https://doi.org/10.1046/j.1365-4362.2000.00749.x
Ffrooz, A., Tehranchia-Nia, Z., & Ahmed, A. R. (1995). Benefits and risks of intralesional corticosteroid injection in the treatment of dermatological diseases. Clinical and Experimental Dermatology, 20(5), 363–370. https://doi.org/10.1111/j.1365-2230.1995.tb01351.x
Fitzpatrick, J., & High, W. (2017). 12 Pustular Eruptions, Non-Follicular. In Urgent Care Dermatology: Symptom-Based Diagnosis (1st ed.). Elsevier.
Fk Islam, Y., & P. Horn, E. (2023). Scleral Discoloration Because of Minocycline Use: A Case Report and Review of the Literature. Military Medicine, 188(3–4), e890–e893. https://doi.org/10.1093/milmed/usab208
Fox, L., Csongradi, C., Aucamp, M., Du Plessis, J., & Gerber, M. (2016). Treatment modalities for acne. Molecules, 21(8), 1063. https://doi.org/10.3390/molecules21081063
Friedlander, S. F., Baldwin, H. E., Mancini, A. J., Yan, A. C., & Eichenfield, L. F. (2011). The acne continuum: An age-based approach to therapy. Seminars in Cutaneous Medicine & Surgery 30(3), S6-11. https://doi.org/10.1016/j.sder.2011.07.002
Gao, J., & Mahto, A. (2016). Anti-Androgen Therapy in Female Adult Acne. Journal of Dermatology Research and Therapy, 2(2), 23. https://doi.org/10.23937/2469-5750/1510023
Garner, S., Eady, A., Bennett, C., Newton, J., Thomas, K., & Popescu, C. (2012). Minocycline for acne vulgaris: Efficacy and safety. Cochrane Database of Systematic Reviews, 8, CD002086. https://doi.org/10.1002/14651858.CD002086.pub2
Giannellis, C. (2023). Topical management strategies of mild acne treatment: An update. AJP: The Australian Journal of Pharmacy, 104(1228), 76–81.
Gollnick, H. (2003). Current Concepts of the Pathogenesis of Acne: Implications for Drug Treatment. Drugs, 63(15), 1579–1596. https://doi.org/10.2165/00003495-200363150-00005
Gollnick, H. P. M. (2015). From new findings in acne pathogenesis to new approaches in treatment. Journal of the European Academy of Dermatology and Venereology, 29(S5), 1–7. https://doi.org/10.1111/jdv.13186
Gollnick, H. P., Zouboulis, C. C., Akamatsu, H., Kurokawa, I., & Schulte, A. (1991). Pathogenesis and pathogenesis related treatment of acne. Journal of Dermatology, 18(9), 489–499. https://doi.org/10.1111/j.1346-8138.1991.tb03122.x
Goodman, L. S. (1996). Goodman and Gilman’s the pharmacological basis of therapeutics (Vol. 1549). McGraw-Hill New York.
Graber, E. M. (2021). Treating acne with the tetracycline class of antibiotics: A review. Dermatological Reviews, 2(6), 321–330. https://doi.org/10.1002/der2.49
Gregoriou, S., Kritsotaki, E., Katoulis, A., & Rigopoulos, D. (2014). Use of tazarotene foam for the treatment of acne vulgaris. Clinical, Cosmetic and Investigational Dermatology, 7, 165–170. https://doi.org/10.2147/CCID.S37327
Greydanus, D., Azmeh, R., Cabral, M., Dickson, C., & Patel, D. (2021). Acne in the first three decades of life: An update of a disorder with profound implications for all decades of life. Disease-a-Month, 67(4), 101103. https://doi.org/10.1016/j.disamonth.2020.101103
Guay, D. R. (2007). Topical Clindamycin in the management of acne vulgaris. Expert Opinion on Pharmacotherapy, 8(15), 2625–2664. https://doi.org/10.1517/14656566.8.15.2625
Guenther, L. C. (2003). Optimizing Treatment with Topical Tazarotene: American Journal of Clinical Dermatology, 4(3), 197–202. https://doi.org/10.2165/00128071-200304030-00006
Guin, J. D. (1981). Treatment of Acne Vulgaris with Topical Clindamycin Phosphate: A Double‐Blind Study. International Journal of Dermatology, 20(4), 286–288. https://doi.org/10.1111/j.1365-4362.1981.tb04339.x
Gupta, M. A., Johnson, A. M., & Gupta, A. K. (1998). The development of an Acne Quality of Life scale: Reliability, validity, and relation to subjective acne severity in mild to moderate acne vulgaris. Acta Dermato-Venereologica, 78(6). https://doi.org/10.1080/000155598442773
Habeshian, K. A., & Cohen, B. A. (2020). Current issues in the treatment of acne vulgaris. Pediatrics, 145(Supplement_2), S225–S230. https://doi.org/10.1542/peds.2019-2056L
Haider, A., & Shaw, J. (2004). Treatment of acne vulgaris. Journal of the American Medical Association, 292(6), 726–735. https://doi.org/10.1001/jama.292.6.726
Handelsman, D. J. (2020). Androgen physiology, pharmacology, use and misuse. Endotext [Internet]. South Dartmouth (MA): MDText.com, Inc.; 2000-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK279000/.
Hazra, M. (2019). A rational pharmacotherapeutic study of comparative safety among topical anti-acne 1% nadifloxacin monotherapy, 0.1% adapalene monotherapy, 0.025% tretinoin monotherapy, 1% nadifloxacin and 0.1% adapalene combination therapy and 1% nadifloxacin and 0.025% tretinoin combination therapy, in mild to moderate acne vulgaris, in tertiary care hospitals. International Journal of Basic & Clinical Pharmacology, 8(9), 1959–1966. https://dx.doi.org/10.18203/2319-2003.ijbcp20193662
Henehan, M., Montuno, M., & De Benedetto, A. (2017). Doxycycline as an anti‐inflammatory agent: Updates in dermatology. Journal of the European Academy of Dermatology and Venereology, 31(11), 1800–1808. https://doi.org/10.1111/jdv.14345
Hess, D. C., & Fagan, S. C. (2010). Repurposing an Old Drug to Improve the Use and Safety of Tissue Plasminogen Activator for Acute Ischemic Stroke: Minocycline. Pharmacotherapy: The Journal of Human Pharmacology and Drug Therapy, 30(7P2). https://doi.org/10.1592/phco.30.pt2.55S
Hirsch, J. G., Chia, P. A., & Jahr, J. S. (2023). Sugammadex: A review of the considerations for women of childbearing age. American Journal of Therapeutics, 30(2), e146–e150. https://doi.org/10.1097/MJT.0000000000001594
Holschbach, M., & Handa, R. (2017). Androgen Action and Stress. In Stress: Neuroendocrinology and Neurobiology (1st ed., Vol. 2, pp. 227–235). Academic Press.
Ibrahim, S., Osman, B., Awaad, R. M., & Abdoon, I. (2023). Acne Vulgaris Relapse in Sudanese Patients Treated with Oral Isotretinoin: Rate and Predictive Factors. Journal of Multidisciplinary Healthcare, 16, 839–849. https://doi.org/10.2147/JMDH.S405509
Ioannides, D., Rigopoulos, D., & Katsambas, A. (2002). Topical adapalene gel 0· 1% vs. isotretinoin gel 0· 05% in the treatment of acne vulgaris: A randomized open-label clinical trial. British Journal of Dermatology, 147(3), 523–527. https://doi.org/10.1046/j.1365-2133.2002.04873.x
Islam, M. R., Baker, M. A., Mondal, N. T., Khan, M. M., & Hossain, M. M. (2023). A Study of the Efficacy of Doxycycline plus Trifarotene in the Treatment of Moderate to Severe Acne Vulgaris. Scholars Journal of Medical Case Reports, 3, 521–529. https://doi.org/10.36347/sjams.2023.v11i03.008
Jain, G. K., & Ahmed, F. J. (2007). Adapalene pretreatment increases follicular penetration of clindamycin: In vitro and in vivo studies. Indian Journal of Dermatology, Venereology and Leprology, 73(5), 326–329. https://doi.org/10.4103/0378-6323.34010
Jain, K., Choudhury, P., Sharma, M., & Dev, S. (2017). Preparation and evaluation of anti-acne herbal gel. European Journal of Biomedical and Pharmaceutical Sciences, 4(10), 578–581.
Johnson, D. B., & Sonthalia, S. (2018). Flutamide. StatPearls [Internet].
Jones, M. C. (2007). Update on Isotretinoin and the iPLEDGE System. US Pharmacist, 32(4), 38.
Jusuf, N. K., Putra, I. B., & Rangkuti, A. D. P. (2023). Assessing acne severity: Teledermatology versus face to face consultations during the COVID-19 pandemic. The Journal of Clinical and Aesthetic Dermatology, 16(1), 30. PMID: 36743968
Kapadia, N., & Talib, A. (2004). Acne treated successfully with azithromycin. International Journal of Dermatology, 43(10), 766–767. https://doi.org/10.1111/j.1365-4632.2004.02058.x
Kardeh, S., Saki, N., Jowkar, F., Kardeh, B., Moein, S. A., & Khorraminejad-Shirazi, M. H. (2019). Efficacy of azithromycin in treatment of acne vulgaris: A mini review. World Journal of Plastic Surgery, 8(2), 127. https://doi.org/10.29252/wjps.8.2.127
Katsambas, A. D., & Dessinioti, C. (2010). Hormonal therapy for acne: Why not as first line therapy? Facts and controversies. Clinics in Dermatology, 28(1), 17–23. https://doi.org/10.1016/j.clindermatol.2009.03.006
Kaya, T. I., Tursen, U., Kokturk, A., & Ikizoglu, G. (2003). An effective extraction technique for the treatment of closed macrocomedones. Dermatologic Surgery, 29(7), 741–744. https://doi.org/10.1046/j.1524-4725.2003.29190.x.
Kazandjieva, J., & Tsankov, N. (2017). Drug-induced acne. Clinics in Dermatology, 35(2), 156–162. https://doi.org/10.1016/j.clindermatol.2016.10.007
Keri, J., & Shiman, M. (2009). An update on the management of acne vulgaris. Clinical, Cosmetic and Investigational Dermatology, 2, 105–110. https://doi.org/10.2147/ccid.s3630
Khaleel, F. F. (2022). Risk factors of acne vulgaris among Mosul University Students from Iraq. Iraqi JMS. 2022; 20 (1): 51-58. doi: 10.22578. Iraqi Journal of Medical Sciences, 20(1), 51–58. https://doi.org/10.22578/IJMS.20.1.7
Khalil, S., Bardawil, T., Stephan, C., Darwiche, N., Abbas, O., Kibbi, A. G., Nemer, G., & Kurban, M. (2017). Retinoids: A journey from the molecular structures and mechanisms of action to clinical uses in dermatology and adverse effects. Journal of Dermatological Treatment, 28(8), 684–696. https://doi.org/10.1080/09546634.2017.1309349
Khunger, N., & Mehrotra, K. (2019). Menopausal Acne – Challenges And Solutions. International Journal of Women’s Health, 11, 555–567. https://doi.org/10.2147/IJWH.S174292
Kim, J. (2005). Review of the innate immune response in acne vulgaris: Activation of Toll-like receptor 2 in acne triggers inflammatory cytokine responses. Dermatology, 211(3), 193–198. https://doi.org/10.1159/000087011
Kim, J. E., Park, A. Y., Lee, S. Y., Park, Y. L., Whang, K. U., & Kim, H.-J. (2018). Comparison of the efficacy of azithromycin versus doxycycline in acne vulgaris: A meta-analysis of randomized controlled trials. Annals of Dermatology, 30(4), 417–426. https://doi.org/10.5021/ad.2018.30.4.417
Kim, K., Jang, H., Kim, E., Kim, H., & Sung, G. Y. (2023). Recent advances in understanding the role of the skin microbiome in the treatment of atopic dermatitis. Experimental Dermatology, 32(12), 2048–2061. https://doi.org/10.1111/exd.14940
Kim, S. Y., & Ochsendorf, F. (2016). New developments in acne treatment: Role of combination adapalene-benzoylperoxide. Therapeutics and Clinical Risk Management, 12, 1497–1506. https://doi.org/10.2147/TCRM.S94062
Kim, W., & Mancini, A. J. (2013). Acne in Childhood: An Update. Pediatric Annals, 42(10), 418–427. https://doi.org/10.3928/00904481-20130924-13
Kircik, L. H. (2013). The role of benzoyl peroxide in the new treatment paradigm for acne. Journal of Drugs in Dermatology, 12(6), s73-6. PMID: 23839205
Kolli, S. S., Pecone, D., Pona, A., Cline, A., & Feldman, S. R. (2019). Topical Retinoids in Acne Vulgaris: A Systematic Review. American Journal of Clinical Dermatology, 20(3), 345–365. https://doi.org/10.1007/s40257-019-00423-z
Krutmann, J., Moyal, D., Liu, W., Kandahari, S., Lee, G.-S., Noppakun, N., Xiang, L. F., & Seité, S. (2017). Pollution and acne: Is there a link? Clinical, Cosmetic and Investigational Dermatology, 10, 199–204. https://doi.org/10.2147/CCID.S131323
Kutlu, Ö. (2020). Effect of isotretinoin treatment on the inflammatory markers in patients with acne vulgaris: Can monocyte/HDL be a new indicator for inflammatory activity of isotretinoin treatment? Cutaneous and Ocular Toxicology, 39(1), 67–70. https://doi.org/10.1080/15569527.2019.1701485
Labib, R., Bury, D., Boisleve, F., Eichenbaum, G., Girard, S., Naciff, J., Leal, M., & Wong, J. (2018). A kinetic-based safety assessment of consumer exposure to salicylic acid from cosmetic products demonstrates no evidence of a health risk from developmental toxicity. Regulatory Toxicology and Pharmacology, 94, 245–251. https://doi.org/10.1016/j.yrtph.2018.01.026
Lavers, I. (2017). Exploring skin anatomy, function and site-specific treatment options. Journal of Aesthetic Nursing, 6(4), 172–180. https://doi.org/10.12968/joan.2017.6.4.172
Layton, A. M., Eady, E. A., Whitehouse, H., Del Rosso, J. Q., Fedorowicz, Z., & Van Zuuren, E. J. (2017). Oral Spironolactone for Acne Vulgaris in Adult Females: A Hybrid Systematic Review. American Journal of Clinical Dermatology, 18(2), 169–191. https://doi.org/10.1007/s40257-016-0245-x
Li, X., He, C., Chen, Z., Zhou, C., Gan, Y., & Jia, Y. (2017). A review of the role of sebum in the mechanism of acne pathogenesis. Journal of Cosmetic Dermatology, 16(2), 168–173. https://doi.org/10.1111/jocd.12345
Lim, S. Y., & Bolster, M. B. (2019). Corticosteroids. In T. A. Cho, S. Bhattacharyya, & S. Helfgott (Eds.), Neurorheumatology (pp. 261–267). Springer International Publishing. https://doi.org/10.1007/978-3-030-16928-2_28
Ly, S., Kamal, K., Manjaly, P., Barbieri, J. S., & Mostaghimi, A. (2023). Treatment of Acne Vulgaris During Pregnancy and Lactation: A Narrative Review. Dermatology and Therapy, 13(1), 115–130. https://doi.org/10.1007/s13555-022-00854-3
Maffeis, L., & Veraldi, S. (2010). Minocycline in the treatment of acne: Latest findings. Giornale Italiano Di Dermatologia e Venereologia, 145(3), 425–429. PMID: 20461050.
Makrantonaki, E., Ganceviciene, R., & Zouboulis, C. C. (2011). An update on the role of the sebaceous gland in the pathogenesis of acne. Dermato-Endocrinology, 3(1), 41–49. https://doi.org/10.4161/derm.3.1.13900
Maleki, A., & Khalid, N. (2018). Exploring the relationship between stress and acne: A medical student’s perspective. Clinical, Cosmetic and Investigational Dermatology, 11, 173–174. https://doi.org/10.2147/CCID.S160985
Malešević, N., Bokan, G., & DJajić, V. (2020). Flutamide induced liver injury in female patients. European Journal of Medical and Health Sciences, 2(5). https://doi.org/10.24018/ejmed.2020.2.5.476
Mancini, A. J., Baldwin, H. E., Eichenfield, L. F., Friedlander, S. F., & Yan, A. C. (2011). Acne life cycle: The spectrum of pediatric disease. Pediatric News, 45(10), S4. https://doi.org/10.1016/j.sder.2011.07.003.
Marks, J., & Miller, J. (2018). 12. Pustules. In Lookingbill and Marks’ Principles of Dermatology (6th ed.).
Marks, R. (2004). Acne and its Management Beyond the Age of 35 Years: American Journal of Clinical Dermatology, 5(6), 459–462. https://doi.org/10.2165/00128071-200405060-00011
Maroñas-Jiménez, L., & Krakowski, A. C. (2016). Pediatric acne: Clinical patterns and pearls. Dermatologic Clinics, 34(2), 195–202. https://doi.org/10.1016/j.det.2015.11.006
Martel, J. L., Miao, J. H., & Badri, T. (2017). Anatomy, hair follicle. StatPearls Publishing, Treasure Island (FL). https://www.ncbi.nlm.nih.gov/books/NBK470321/
Martins, A., Marto, J., Johnson, A., & Graber, E. (2021). A Review of Systemic Minocycline Side Effects and Topical Minocycline as a Safer Alternative for Treating Acne and Rosacea. Antibiotics, 10(7), 757. https://doi.org/10.3390/antibiotics10070757
McLaughlin, J., Watterson, S., Layton, A. M., Bjourson, A. J., Barnard, E., & McDowell, A. (2019). Propionibacterium acnes and acne vulgaris: New insights from the integration of population genetic, multi-omic, biochemical and host-microbe studies. Microorganisms, 7(5), 128. https://doi.org/10.3390/microorganisms7050128
McNeil, M. P., Luthy, K. E., Platt, C. R., Robinson, M. S., & Macintosh, J. L. (2023). First-Line Acne Treatment: Efficacy and Comparison of Cost. The Journal for Nurse Practitioners, 19(6), 104616. https://doi.org/10.1016/j.nurpra.2023.104616
Mehra, T., Borelli, C., Burgdorf, W., Röcken, M., & Schaller, M. (2012). Treatment of severe acne with low-dose isotretinoin. Acta Dermato-Venereologica, 92(3), 247–248. https://doi.org/ 10.2340/00015555-1325
Mohiuddin, A. (2019). A comprehensive review of acne vulgaris. Journal of Clinical Pharmacy, 1(1), 17–45. http://innovationinfo.org/articles/JCP/JCP-103.pdf
Mollerup, S., Friis-Nielsen, J., Vinner, L., Hansen, T. A., Richter, S. R., Fridholm, H., Herrera, J. A. R., Lund, O., Brunak, S., Izarzugaza, J. M. G., Mourier, T., Nielsen, L. P., & Hansen, A. J. (2016). Propionibacterium acnes: Disease-Causing Agent or Common Contaminant? Detection in Diverse Patient Samples by Next-Generation Sequencing. Journal of Clinical Microbiology, 54(4), 980–987. https://doi.org/10.1128/JCM.02723-15
Montagna, W. (2012). The structure and function of skin. Elsevier. https://www.sciencedirect.com/book/monograph/9780125052634/the-structure-and-function-of-skin
Moradi Tuchayi, S., Alexander, T., Nadkarni, A., & Feldman, S. R. (2016). Interventions to increase adherence to acne treatment. Patient Preference and Adherence, 10, 2091–2096. https://doi.org/10.2147/PPA.S117437
Mossman, J. (2006). Preventing and treating acne. US Pharmacist, 31(4), 34–42.
Munir, S., Fathima, R., Melath, A., Kayakool, S., & Arjun, M. (2023). The Chemical Essence of life Antibiotics. Journal of Dental Science Research Reviews & Reports, 5(1), 1–13. https://doi.org/doi.org/10.47363/JDSR/2023(5)146
Nassar, A. A. E. R., Ibrahim, A. M., & Youssef, A. G. (2023). New Management Lines of Acne Vulgaris. The Egyptian Journal of Hospital Medicine, 91(1), 4152–4157.
Nelson, M. L., & Levy, S. B. (2011). The history of the tetracyclines. Annals of the New York Academy of Sciences, 1241(1), 17–32. https://doi.org/10.1111/j.1749-6632.2011.06354.x
Newman, M. D., Bowe, W. P., Heughebaert, C., & Shalita, A. R. (2011). Therapeutic Considerations for Severe Nodular Can.: American Journal of Clinical Dermatology, 12(1), 7–14. https://doi.org/10.2165/11532280-000000000-00000
NilFroushzadeh, M. A., Siadat, A. H., Baradaran, E. H., & Moradi, S. (2009). Clindamycin lotion alone versus combination lotion of clindamycin phosphate plus tretinoin versus combination lotion of clindamycin phosphate plus salicylic acid in the topical treatment of mild to moderate acne vulgaris: A randomized control trial. Indian Journal of Dermatology, Venereology and Leprology, 75(3), 279–282. https://doi.org/10.4103/0378-6323.51247.
Noor, A., & Khetarpal, S. (2024). Anaerobic infections. StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing.
Olisova, O. Y., & Anpilogova, E. M. (2023). Clindamycin/benzoyl peroxid gel in mild-to-moderate acne. Vestnik Dermatologii i Venerologii, 99(1), 55–61. https://doi.org/10.25208/vdv1370
Otlewska, A., Baran, W., & Batycka-Baran, A. (2020). Adverse events related to topical drug treatments for acne vulgaris. Expert Opinion on Drug Safety, 19(4), 513–521. https://doi.org/10.1080/14740338.2020.1757646
Pappas, A., Johnsen, S., Liu, J.-C., & Eisinger, M. (2009). Sebum analysis of individuals with and without acne. Dermato-Endocrinology, 1(3), 157–161. https://doi.org/10.4161/derm.1.3.8473
Parwez, S., Zainab, S. R., & Andaleeb, S. (2023). Self-Esteem And Social Anxiety Among Face Acne Patients In Peshawar. Multicultural Education, 9(3). https://doi.org/10.5281/zenodo.7719384
Patel, D. J., & Bhatia, N. (2021). Oral Antibiotics for Acne. American Journal of Clinical Dermatology, 22(2), 193–204. https://doi.org/10.1007/s40257-020-00560-w
Pazos, F., Escobar-Morreale, H. F., Balsa, J., Sancho, J. M., & Varela, C. (1999). Prospective randomized study comparing the long-acting gonadotropin-releasing hormone agonist triptorelin, flutamide, and cyproterone acetate, used in combination with an oral contraceptive, in the treatment of hirsutism. Fertility and Sterility, 71(1), 122–128. https://doi.org/10.1016/s0015-0282(98)00414-2.
Pedro-Hernández, L. D., Martínez-Klimova, E., Martínez-Klimov, M. E., Cortez-Maya, S., Vargas-Medina, A. C., Ramírez-Ápan, T., Hernández-Ortega, S., & Martínez-García, M. (2018). Anticancer activity of resorcinarene-PAMAM-dendrimer conjugates of flutamide. Anti-Cancer Agents in Medicinal Chemistry (Formerly Current Medicinal Chemistry-Anti-Cancer Agents), 18(7), 993–1000. https://doi.org/10.2174/1871520618666171219114532
Perche, P. O., Peck, G. M., Robinson, L., Grada, A., Fleischer Jr, A. B., & Feldman, S. R. (2023). Prescribing trends for acne vulgaris visits in the United States. Antibiotics, 12(2), 269. https://doi.org/10.3390/antibiotics12020269
Perry, A., & Lambert, P. (2011). Propionibacterium acnes: Infection beyond the skin. Expert Review of Anti-Infective Therapy, 9(12), 1149–1156. https://doi.org/10.1586/eri.11.137
Piquero‐Casals, J., Morgado‐Carrasco, D., Rozas‐Muñoz, E., Mir‐Bonafé, J. F., Trullàs, C., Jourdan, E., Piquero‐Martin, J., Zouboulis, C. C., & Krutmann, J. (2023). Sun exposure, a relevant exposome factor in acne patients and how photoprotection can improve outcomes. Journal of Cosmetic Dermatology, 22(6), 1919–1928. https://doi.org/10.1111/jocd.15726
Plewig, G., & Kligman, A. M. (2012). Acne: Morphogenesis and treatment. Springer Science & Business Media.
Polak‐Witka, K., Rudnicka, L., Blume‐Peytavi, U., & Vogt, A. (2020). The role of the microbiome in scalp hair follicle biology and disease. Experimental Dermatology, 29(3), 286–294. https://doi.org/10.1111/exd.13935
Preneau, S., & Dreno, B. (2012). Female acne – a different subtype of teenager acne? Journal of the European Academy of Dermatology and Venereology, 26(3), 277–282. https://doi.org/10.1111/j.1468-3083.2011.04214.x
Pugashetti, R., & Shinkai, K. (2013). Treatment of acne vulgaris in pregnant patients: Treatment of acne vulgaris in pregnant patients. Dermatologic Therapy, 26(4), 302–311. https://doi.org/10.1111/dth.12077
Raine, S. P. (2023). Legal and Ethical Issues in the Neurology of Reproductive Health. Neurologic Clinics, 41(3), 533–541. https://doi.org/10.1016/j.ncl.2023.03.003
Rajar, U. D. M., Mashhood, A. A., Fahim, A., Kazi, N., & Hanif, M. (2023). Comparing the effects of isotretinoin 20 mg versus azithromycin 500 mg in the management of acne vulgaris: A randomized clinical trial. International Journal of Dermatology, 62(8), 1082–1087. https://doi.org/10.1111/ijd.16615
Ramos, P. M., Melo, D. F., Radwanski, H., Almeida, R. F. C. de, & Miot, H. A. (2023). Female-pattern hair loss: Therapeutic update. Anais Brasileiros de Dermatologia, 98(4), 506–519. https://doi.org/10.1016/j.abd.2022.09.006
Rao, P. K., Bhat, R. M., Nandakishore, B., Dandakeri, S., Martis, J., & Kamath, G. H. (2014). Safety and efficacy of low-dose isotretinoin in the treatment of moderate to severe acne vulgaris. Indian Journal of Dermatology, 59(3), 316. https://doi.org/10.4103/0019-5154.131455
Rathi, S. K. (2011). Acne vulgaris treatment: The current scenario. Indian Journal of Dermatology, 56(1), 7–13. https://doi.org/10.4103/0019-5154.77543
Ravisankar, P., Koushik, O. S., Himaja, V., Ramesh, J., & Pragna, P. (2015). Acne-causes and amazing remedial measures for acne. Indo American Journal of Pharmaceutical Research, 5(7), 209–301.
Roberts, E. E., Nowsheen, S., Davis, D. M. R., Hand, J. L., Tollefson, M. M., & Wetter, D. A. (2021). Use of spironolactone to treat acne in adolescent females. Pediatric Dermatology, 38(1), 72–76. https://doi.org/10.1111/pde.14391
Rosenthal, S. A., Linstadt, D. E., Leibenhaut, M. H., Andras, E. J., Brooks, C. P., Stickney, D. R., Chang, G. C., Wolkov, H. B., & Gilbert, R. M. (1996). Flutamide-associated liver toxicity during treatment with total androgen suppression and radiation therapy for prostate cancer. Radiology, 199(2), 451–455. https://doi.org/10.1148/radiology.199.2.8668793
Rouse, J. G., & Van Dyke, M. E. (2010). A review of keratin-based biomaterials for biomedical applications. Materials, 3(2), 999–1014. https://doi.org/10.3390/ma3020999
Ruchiatan, K., Rahardja, J. I., Rezano, A., Hindritiani, R., Sutedja, E., & Gunawan, H. (2020). A five-year clinical acne patients profiles and its management based on Indonesian acne expert guideline in Bandung, Indonesia. Journal of Pakistan Association of Dermatologists, 30(2), 229–234.
Rumsfield, J. A., West, D. P., Tse, C. S. T., Eaton, M. L., & Robinson, L. A. (1983). Isotretinoin in Severe, Recalcitrant Cystic Acne: A Review. Drug Intelligence & Clinical Pharmacy, 17(5), 329–333. https://doi.org/10.1177/106002808301700502
Russell, J. J. (2000). Topical therapy for acne. American Family Physician, 61(2), 357–365.
Sadati, M. S., Yazdanpanah, N., Shahriarirad, R., Javaheri, R., & Parvizi, M. M. (2023). Efficacy of metformin vs. doxycycline in treating acne vulgaris: An assessor‐blinded, add‐on, randomized, controlled clinical trial. Journal of Cosmetic Dermatology, 22(10), 2816–2823. https://doi.org/10.1111/jocd.15785
Sagar, T. V., & Kumar, S. (2023). Safety and efficacy of nadifloxacin versus clindamycin observed in a tertiary care teaching hospital of Deccan Plateau. Indian Journal of Pharmacy and Pharmacology, 10(1), 24–27. https://doi.org/10.18231/j.ijpp.2023.007
Sagransky, M., Yentzer, B. A., & Feldman, S. R. (2009). Benzoyl peroxide: A review of its current use in the treatment of acne vulgaris. Expert Opinion on Pharmacotherapy, 10(15), 2555–2562. https://doi.org/10.1517/14656560903277228
Saleem, S., Raza, N., Saleem, N., Ullah, S., Yasmin, G., & Yousaf, F. (2023). Efficacy of Topical 0.05% Isotretinoin Gel Versus 0.1% Adapalene Gel in The Treatment of Mild to Moderate Acne Vulgaris. Pakistan Armed Forces Medical Journal, 73(1), 107–110. https://doi.org/10.51253/pafmj.v73i1.6472
Sanghvi, A. (2022). Bumps on Arms: Treatment, Home Remedies, and Self-Care Tips. Emedihealth. https://www.emedihealth.com/skin-beauty/more-skin-conditions/manage-bumps-on-arms
Sanjel, K., & Zhang, X. M. (2022). Progress of different treatment modalities to limit the use of antibiotics in the treatment of acne. Our Dermatology Online/Nasza Dermatologia Online, 13(1), 92–97. https://doi.org/10.7241/ourd.20221.23
Sanke, S., Chander, R., & Mehra, S. (2019). Intralesional radiofrequency for papular acne scars. Indian Dermatology Online Journal, 10(4), 486–487. https://doi.org/10.4103/idoj.IDOJ_75_19
Sanshita, R. B., Sood, P., Thakur, D., & Kuhad, A. (2023). Repurposing of Minocycline, a Tetracycline Antibiotic, for Neurodegenerative Disorders. In R. C. Sobti, S. K. Lal, & R. K. Goyal (Eds.), Drug Repurposing for Emerging Infectious Diseases and Cancer (pp. 615–654). Springer Nature Singapore. https://doi.org/10.1007/978-981-19-5399-6_27
Savage, L. J., & Layton, A. M. (2010). Treating acne vulgaris: Systemic, local and combination therapy. Expert Review of Clinical Pharmacology, 3(4), 563–580. https://doi.org/10.1586/ecp.10.27
Say, Y.-H., Heng, A. H. S., Reginald, K., Wong, Y. R., Teh, K. F., Rawanan Shah, S. M., Sio, Y. Y., Ng, Y. T., Matta, S. A., Pang, S. L., & Chew, F. T. (2021). Modifiable and non-modifiable epidemiological risk factors for acne, acne severity and acne scarring among Malaysian Chinese: A cross-sectional study. BMC Public Health, 21(1), 601. https://doi.org/10.1186/s12889-021-10681-4
Sayyafan, M. S., Ramzi, M., & Salmanpour, R. (2020). Clinical assessment of topical erythromycin gel with and without zinc acetate for treating mild-to-moderate acne vulgaris. Journal of Dermatological Treatment, 31(7), 730–733. https://doi.org/10.1080/09546634.2019.1606394
Schrager, S., Larson, M., Carlson, J., Ledford, K., & Ehrenthal, D. B. (2020). Beyond Birth Control: Noncontraceptive Benefits of Hormonal Methods and Their Key Role in the General Medical Care of Women. Journal of Women’s Health, 29(7), 937–943. https://doi.org/10.1089/jwh.2019.7731
Shaw, J. C. (1991). Spironolactone in dermatologic therapy. Journal of the American Academy of Dermatology, 24(2), 236–243. https://doi.org/10.1016/0190-9622(91)70034-Y
Silverberg, N. (2023). Skin Deep: A Dermatologist’s Guide to the Science of Skin Care. Archway Publishing.
Simonart, T., & Dramaix, M. (2005). Treatment of acne with topical antibiotics: Lessons from clinical studies. British Journal of Dermatology, 153(2), 395–403. https://doi.org/10.1111/j.1365-2133.2005.06614.x
Skidgel, R. A., & Erdos, E. G. (2016). Histamine, bradykinin, and their antagonists. In: Hilal-Dandan R, Brunton LL. eds. Goodman and Gilman’s Manual of Pharmacology and Therapeutics. McGraw-Hill Education.
Skinacea. (2012). How to Apply a “Pea-Sized” Amount. Skinacea. https://www.skinacea.com/how-to/apply-pea-sized-amount.html
Spencer, E. H., Ferdowsian, H. R., & Barnard, N. D. (2009). Diet and acne: A review of the evidence. International Journal of Dermatology, 48(4), 339–347. https://doi.org/10.1111/j.1365-4632.2009.04002.x
Suárez-Rivero, J. M., López-Pérez, J., Muela-Zarzuela, I., Pastor-Maldonado, C., Cilleros-Holgado, P., Gómez-Fernández, D., Álvarez-Córdoba, M., Munuera-Cabeza, M., Talaverón-Rey, M., & Povea-Cabello, S. (2023). Neurodegeneration, mitochondria, and antibiotics. Metabolites, 13(3), 416. https://doi.org/10.3390/metabo13030416
Suva, M. A., Patel, A. M., Sharma, N., Bhattacharya, C., & Mangi, R. K. (2014). A brief review on acne vulgaris: Pathogenesis, diagnosis and treatment. Research & Reviews: Journal of Pharmacology, 4(3), 1–12.
Tabri, F., Patellongi, I., Wahab, S., & Djawad, K. (2017). Analysis of nutritional status and levels of sebum on various age groups. American Journal of Clinical and Experimental Medicine, 5(1), 26–29. https://doi.org/10.11648/j.ajcem.20170501.16
Takata, K., & Hirai, F. (2023). Minocycline-induced black hairy tongue and skin hyperpigmentation. BMJ Case Reports, 16(4), e253811. https://doi.org/10.1136/bcr-2022-253811
Tan, A. U., Schlosser, B. J., & Paller, A. S. (2018). A review of diagnosis and treatment of acne in adult female patients. International Journal of Women’s Dermatology, 4(2), 56–71. https://doi.org/10.1016/j.ijwd.2017.10.006
Tanghetti, E. (2013). The role of inflammation in the pathology of acne. The Journal of clinical and aesthetic dermatology. The Journal of Clinical and Aesthetic Dermatology, 6(9), 27–35. PMID: 24062871
Thomson, K. F., Goulden, V., Sheehan-Dare, R., & Cunliffe, W. J. (1999). Light cautery of macrocomedones under general anaesthesia. British Journal of Dermatology, 141(3), 595–596. https://doi.org/10.1046/j.1365-2133.1999.03083.x
Titus, S., & Hodge, J. (2012). Diagnosis and treatment of acne. American Family Physician, 86(8), 734–740.
Tolaymat, L., Dearborn, H., & Zito, P. M. (2023). Adapalene. In StatPearls [Internet]. StatPearls Publishing.
Tripathi, S. V., Gustafson, C. J., Huang, K. E., & Feldman, S. R. (2013). Side effects of common acne treatments. Expert Opinion on Drug Safety, 12(1), 39–51. https://doi.org/10.1517/14740338.2013.740456
Trivedi, M. K., Shinkai, K., & Murase, J. E. (2017). A Review of hormone-based therapies to treat adult acne vulgaris in women. International Journal of Women’s Dermatology, 3(1), 44–52. https://doi.org/10.1016/j.ijwd.2017.02.018
Tucker, R., & Walton, S. (2007). The role of benzoyl peroxide in the management of acne vulgaris. Pharmaceutical Journal, 279(7460), 48–53.
Ullah, G., Noor, S. M., Bhatti, Z., Ahmad, M., & Bangash, A. R. (2014). Comparison of oral azithromycin with oral doxycycline in the treatment of acne vulgaris. Journal of Ayub Medical College Abbottabad, 26(1), 64–67. PMID: 25358221.
Uslar, T., Olmos, R., Martínez-Aguayo, A., & Baudrand, R. (2023). Clinical update on congenital adrenal hyperplasia: Recommendations from a multidisciplinary adrenal program. Journal of Clinical Medicine, 12(9), 3128. https://doi.org/10.3390/jcm12093128
Van Onselen, J. (2011). Scalp problems in eczema. Journal of Community Nursing, 25(1), 10–13.
Varghese, K., Dykstra, J., & Bisbee, E. (2023). Minocycline-Induced Hyperpigmentation of Nails. Cureus, 15(5), e38640. https://doi.org/10.7759/cureus.38640
Vasam, M., Korutla, S., & Bohara, R. A. (2023). Acne vulgaris: A review of the pathophysiology, treatment, and recent nanotechnology based advances. Biochemistry and Biophysics Reports, 36, 101578. https://doi.org/10.1016/j.bbrep.2023.101578
Vedamurthy, M. (2004). Salicylic acid peels. Indian Journal of Dermatology, Venereology & Leprology, 70(2), 136–138. PMID: 17642590.
Vedamurthy, M. (2023). Topical anti-acne agents. In Essentials for Aesthetic Dermatology in Ethnic Skin (pp. 108–112). CRC Press.
Vichare, V., Handargule, P., Tambe, V., Dhole, S., & Choudhari, V. (2023). Identification of Oxidative Degradation Products of Dapsone in Presence of Adapalene by RP-HPLC–MS. Chromatographia, 86, 223–235. https://doi.org/10.1007/s10337-023-04234-7
Villani, A., Nastro, F., Di Vico, F., Fabbrocini, G., Annunziata, M. C., & Genco, L. (2022). Oral isotretinoin for acne: A complete overview. Expert Opinion on Drug Safety, 21(8), 1027–1037. https://doi.org/10.1080/14740338.2022.2102605
Walsh, T. R., Efthimiou, J., & Dréno, B. (2016). Systematic review of antibiotic resistance in acne: An increasing topical and oral threat. The Lancet Infectious Diseases, 16(3), e23–e33. . https://doi.org/10.1016/S1473-3099(15)00527-7.
Wan, S. (2015). The cause and treatment of acne vulgaris: Fact versus fiction [Master’s Thesis, Boston University]. https://hdl.handle.net/2144/13948
Wang, Y., Kuo, S., Shu, M., Yu, J., Huang, S., Dai, A., Two, A., Gallo, R. L., & Huang, C.-M. (2014). Staphylococcus epidermidis in the human skin microbiome mediates fermentation to inhibit the growth of Propionibacterium acnes: Implications of probiotics in acne vulgaris. Applied Microbiology and Biotechnology, 98(1), 411–424. https://doi.org/10.1007/s00253-013-5394-8
Wang, Y., Su, J., Zhou, Z., Yang, J., Liu, W., Zhang, Y., Zhang, P., Guo, T., & Li, G. (2023). Baicalein Resensitizes Multidrug-Resistant Gram-Negative Pathogens to Doxycycline. Microbiology Spectrum, 11(3), e04702-22. https://doi.org/10.1128/spectrum.04702-22
Webster, G. F., Poyner, T., & Cunliffe, B. (2002). Clinical review Acne vulgaris Commentary: A UK primary care perspective on treating acne. British Medical Journal, 325(7362), 475–479. https://doi.org/10.1136/bmj.325.7362.475
Woźniacka, A., Czuwara, J., Krasowska, D., Chlebus, E., Wąsik, G., Wojas-Pelc, A., Rudnicka, L., Narbutt, J., Adamski, Z., & Czajkowski, R. (2022). Rosacea–diagnostic and therapeutic recommendations of the Polish Dermatological Society. Part 2. Treatment. Dermatology Review/Przegląd Dermatologiczny, 109(6), 397–416. https://doi.org/10.5114/dr.2022.126600
Yang, J., Yang, H., Xu, A., & He, L. (2020). A review of advancement on influencing factors of acne: An emphasis on environment characteristics. Frontiers in Public Health, 8, 450. https://doi.org/10.3389/fpubh.2020.00450
Yasin, M. A. N. M. S. (2015). Treatment and Management of Acne. Journal of Pharmacy and Alternative Medicine, 8, 1-7.
Yoham, A. L., & Casadesus, D. (2020). Tretinoin. StatPearls Publishing, Treasure Island (FL), PMID: 32491410.
Zakaria, A. S. M., Paul, H. K., Rahman, M. A., Islam, M. T., & Choudhury, A. M. (2010). Topical tazarotene cream (0.1%) in the treatment of facial acne: An open clinical trial. Bangladesh Medical Research Council Bulletin, 36(2), 43–46. https://doi.org/10.3329/bmrcb.v36i2.6985
Zhang, P., Tian, L., Bao, J., Li, S., Li, A., Wen, Y., Wang, J., & Jie, Y. (2022). Isotretinoin impairs the secretory function of meibomian gland via the PPARγ signaling pathway. Investigative Ophthalmology & Visual Science, 63(3), 29–29. https://doi.org/10.1167/iovs.63.3.29
Zouboulis, C. C., & Rabe, T. (2010). Hormonal antiandrogens in acne treatment. Journal Der Deutschen Dermatologischen Gesellschaft, 8, S60-74. https://doi.org/10.1111/j.1610-0387.2009.07171.x